By Laila A. Bell
The foundation for lifelong health is laid during the early years. In order for children to enjoy their best health during adulthood they need a healthy start in life, routine preventive care, and homes and communities equipped with the resources that support healthy lifestyles.
The latest North Carolina Child Health Report Card finds two bookends for child health in North Carolina. There’s good news in the report: we’ve made impressive gains in a key area that promotes child health. Yet the report also finds North Carolina’s failure to address a significant public health challenge has limited other progress. In both cases, good and bad, it’s clear that public policy decisions have a dramatic impact on the lives of our state’s children.
Where are we doing well?
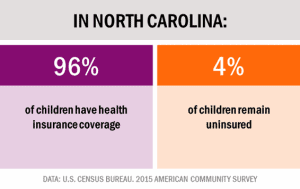
A historic percentage of North Carolina children have health insurance coverage, which is an essential first step on the road to enabling children to access preventive and medical care that promotes good health. Since 2009, the percentage of uninsured children in North Carolina has declined by half to reach a record low of 4 percent.
Children’s health insurance coverage is strengthened by Medicaid, NC Health Choice– the state’s Children’s Health Insurance Program–as well as the Affordable Care Act. Together, these programs complement private market participation and increase insurance coverage to 96 percent of all children in North Carolina. The majority of all children in the state (53 percent) receive their coverage through Medicaid and NC Health Choice which are federally funded programs that are administered at the state level.
Congress is currently pursuing changes to the Medicaid program that would radically restructure it by capping the amount of money available to states. If enacted, previous estimates have shown these changes could reverse improvements in children’s health insurance coverage and result in North Carolina children losing their insurance coverage.
The consequences of the federal debate about health reform could be especially dire for children with special needs and disabilities, who compose nearly one in every five children in the state (17.2 percent).* A capped Medicaid program would eliminate or weaken the long-standing guarantee that all children enrolled in Medicaid receive medically-necessary screenings and treatments, even expensive (and life-saving) services for medically-fragile children. The federal government facilitated state compliance with this provision by providing matching funds for needed services. If the current bill passes and funding to states is capped, North Carolina will lack the financial resources to pay for needed services and treatments, leaving the most vulnerable children exposed to deep cuts in health care.
Where can we improve?
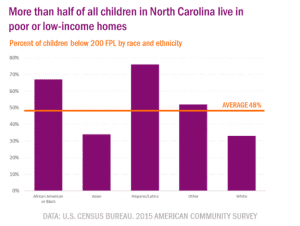
North Carolina received an ‘F’ for economic security. This is the first time since 2010 that the data for a measure was so severe that it earned the lowest possible grade from our panel of health experts. Half of all children in North Carolina (48 percent), and more than half of the youngest children in our state (55 percent), live in poor or near poor homes. When we examine the data by race and ethnicity the findings are shocking: more than two-thirds of our African American children and three-quarters of our Hispanic or Latinx children live in homes that experience significant barriers to good health.
Income influences health status and outcomes. The greater one’s income, the lower the likelihood of disease or even premature death. Children in poverty are more than nine times as likely to be in fair or poor health than their peers who lives in homes with incomes greater than 400 percent of the federal poverty line. Research also finds that differences in income contribute to the alarming racial and ethnic disparities we observe in many of the other indicators in this year’s report.
How do we get there?
This tale of two indicators weaves a compelling narrative about the impact of public investments in child health. When we identify, prioritize, and invest in removing obstacles to child health–as we have with uninsurance rates–we can measurably improve the well-being of children today and dramatically alter the trajectory of their lives. However, when we fail to prioritize and take action on key child well-being challenges–as we have with poverty–our children bear the consequences through poorer health and diminished future opportunities.
*National Survey of Children with Special Health Care Needs, Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Bureau. Available online at: http://childhealthdata.org/browse/survey/results?q=1792&r=35